How limited broadband affects older adults during COVID-19
Consistent data shows us that people over the age of 60 are at the highest risk for severe health problems relating to COVID-19.
Unfortunately, this subset of the population, especially those living in rural areas, have had their medical needs grossly underserved since long before this national health crisis emerged. Older adults living in rural communities don’t have the same access to medical care as those living in more urban and connected areas.
With a dramatic rise in rural hospital closures since 2010, and poor broadband infrastructure unable to support modern telehealth solutions, we as a nation are failing to protect aging rural Americans.
Those who’ve contracted COVID-19, in addition to those who have ongoing-unrelated medical needs, must make the impossible decision to either expose themselves to the novel coronavirus at their nearest hospital (often more than 40 minutes away) or decline necessary medical care in order to avoid exposure.
This poses a serious challenge — but one that could be alleviated through the expansion of telehealth solutions, which allow the most vulnerable older Americans to access care remotely without exposing themselves to disease.
However, in many rural areas, lack of broadband availability makes telehealth impossible. To visualize the challenges that rural areas face — and to find where telehealth could potentially become a solution—we built a map overlaying hospital coverage and broadband access.
A national health crisis
As the number of people infected with COVID-19 increases by the day, the nation watches anxiously as new cases and hotspots extend across the country. Spreading from major metropolises to small towns and communities, the virus proves it doesn’t discriminate by geography. It does however, appear to be taking the greatest toll on older Americans, a group that is overrepresented in rural America.
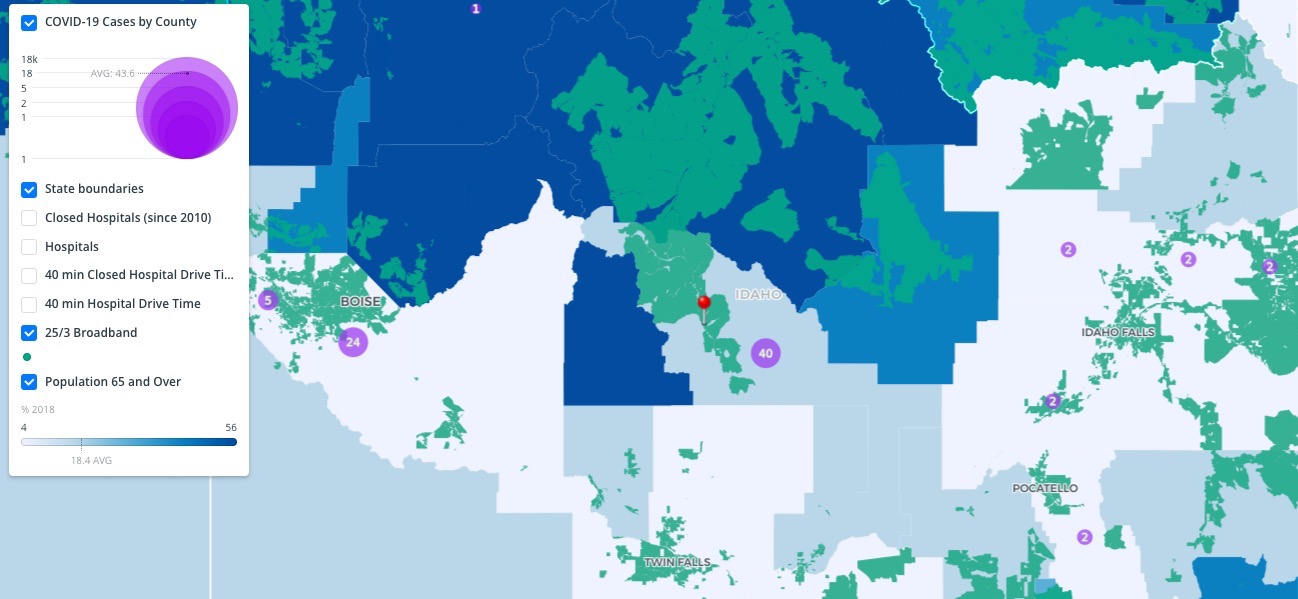
A look at the growing number of confirmed COVID-19 cases (updated in real time):
A disconnected nation
During unprecedented health crises like the one we face today, older Americans can often be best served by using telehealth solutions to consult with healthcare providers virtually from the comfort (and safety) of their own homes. This way, they eliminate the risk of disease exposure at a clinic or a hospital. Unfortunately, because telehealth is only an option where there is broadband availability, the millions of rural Americans who lack broadband access are often left disconnected and underserved.
A look at where a lack of broadband availability stifles telehealth opportunities for aging rural Americans:
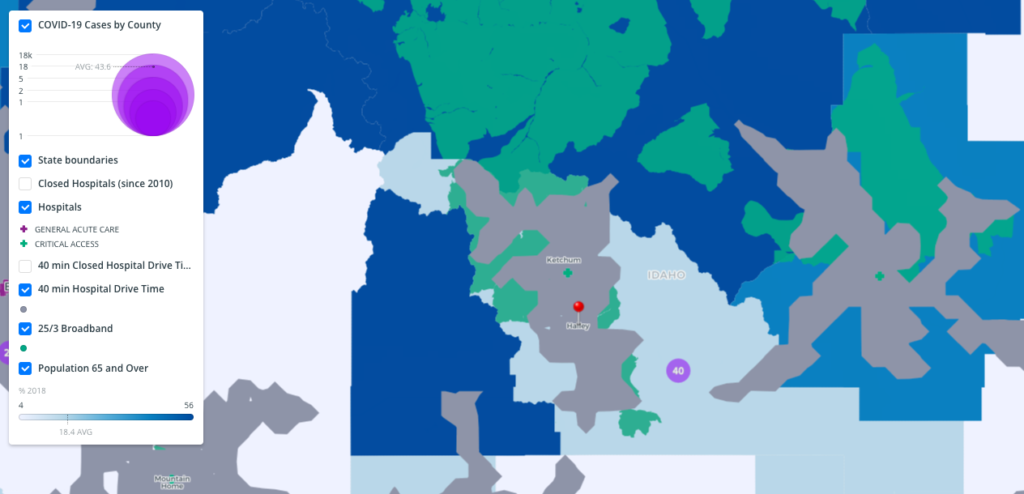
An impossible situation
This is particularly difficult in rural areas of the country with hospital deserts.
Older rural Americans, both those with COVID-19 symptoms and those without, lack safe medical solutions. Many are left with the choice to either drive more than 40 minutes to care facilities that put them at risk, or to stay home and not receive treatment. A quarter of rural Americans who say they are unable to get the care they need cite distance to a provider as their primary obstacle.
A look at the distance aging rural Americans must travel for basic health care needs:
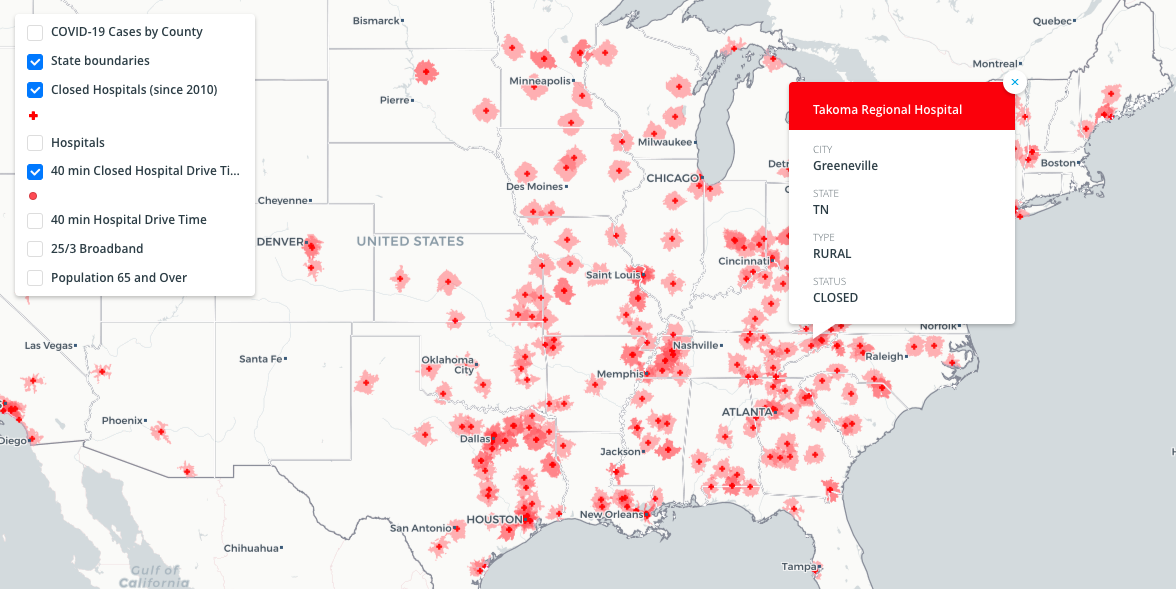
A changing landscape
Since 2010, more than 126 hospitals have closed in rural areas of the country. This is a real crisis that has severely worsened rural health outcomes.
These consequences have long been apparent — of all regions of the country, rural areas face the lowest life expectancy, highest mortality rates, and increased risk for cancer, heart disease, suicide, and opioid addiction. However, while hospital closures pose a real threat, there are ways to alleviate the gap that they cause.
A look at health care gaps and where hospitals have closed since 2010:
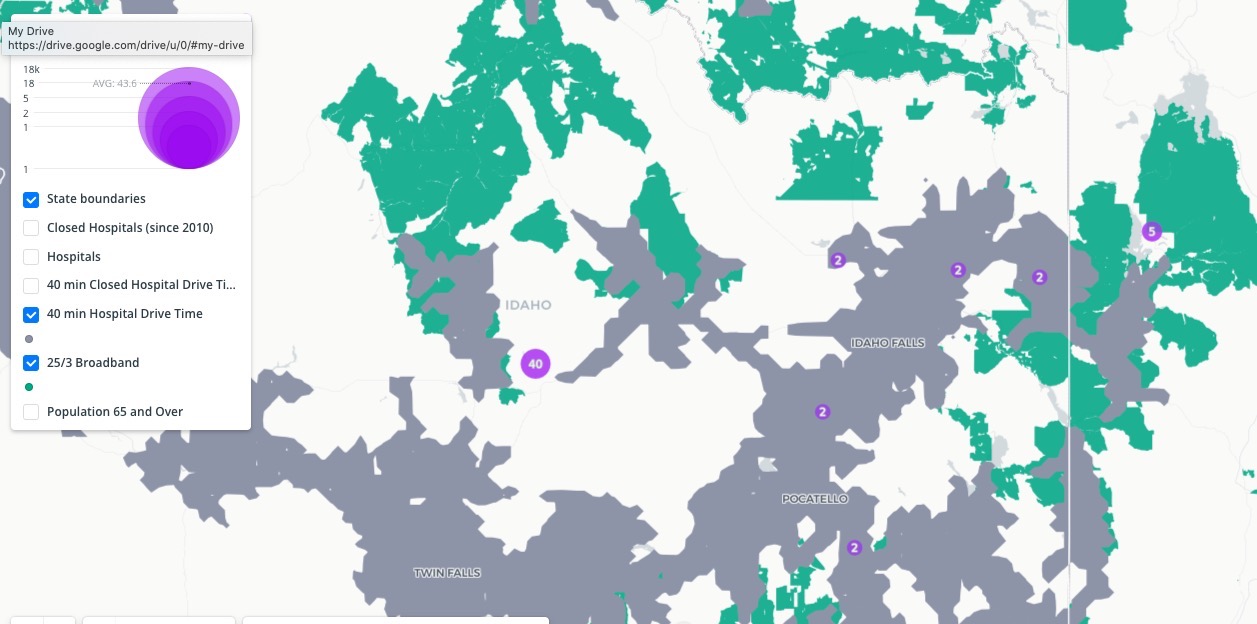
A future-proof approach
The places where health care gaps and broadband exist synchronously are ideal places to prioritize the deployment of telehealth services that can serve the populations that live there. This reduces the risk for aging rural Americans who need both COVID-19 and non-COVID-19 medical attention while also taking pressure off of hospital facilities and staff.
A look at rural communities where there are both health care gaps and broadband availability:
The COVID-19 pandemic has made rural health care gaps painfully obvious. While the virus will likely get worse before it gets better, we must identify rural areas with broadband availability that can expand telehealth access and provide equitable health care solutions for all Americans. To learn more about our mapping and data analytics work, or to request a map you’d like to see, please don’t hesitate to send us an email.
To learn more about the data sets we’ve used to build this map, please view our codebook below.